Outsource revenue cycle management to Connexus Cure and maximize your practice’s revenue with accuracy, transparency, and full compliance.
Revenue Cycle Management Services in Alaska (AK)
Connexus offers complete Revenue Cycle Management (RCM) services in Alaska (AK). These services are designed to increase your practice’s revenue, decrease administrative work, and guarantee compliance. Our services cover every part of the revenue cycle, from scheduling appointments to collecting payments. This allows you to concentrate on patient care while we manage your practice’s revenue cycle.
What is Revenue Cycle Management ?
Revenue Cycle Management (RCM) is the complete financial process that healthcare practices use to manage all the revenue of their practice. It starts when a patient shedules an appointment. It includes insurance verification, medical coding, charge capture, claims submission, payment processing, denial management, and patient collections. The goal of healthcare revenue cycle management is ensure accurate billing, timely payments, reduced claim denials, regulatory compliance & improved cash flow for all medical practices such as hospitals, clinics & healthcare organizations.
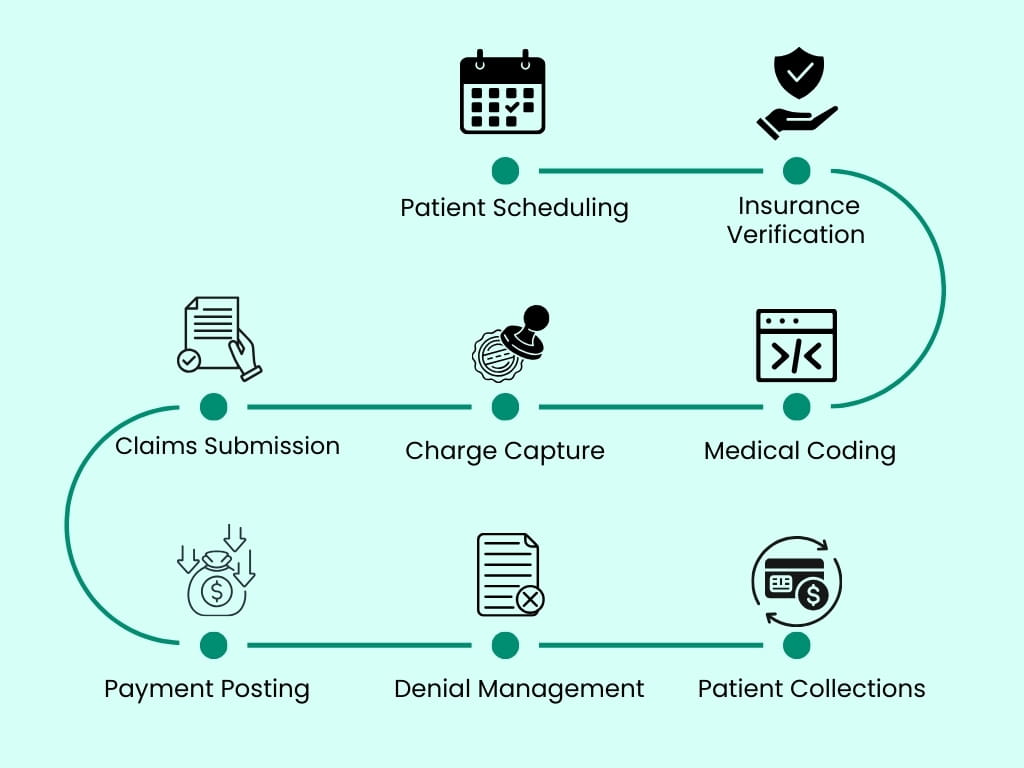
End-to-End Revenue Cycle Management Services in Alaska
We provide comprehensive healthcare revenue cycle management services in Alaska (AK) designed to increase collections, reduce denials & improve financial performance for hospitals, clinics, healthcare organizations.
Our team verifies patient demographics, insurance coverage, prior authorizations, and benefits before the visit to prevent costly claim rejections.
What We Deliver:
➤ Real-time eligibility verification
➤ Benefits & coverage confirmation
➤ Prior authorization management
➤ Reduced front-end claim errors
Result: Fewer denials & faster reimbursements.
Our certified coding specialists ensure correct CPT, ICD-10 & HCPCS coding while maintaining strict compliance with payer & regulatory guidelines.
What We Deliver:
➤ Certified professional coders (CPC)
➤ Specialty-specific coding expertise
➤ Compliance-focused documentation review
➤ Clean claim submission
Result: Maximized Revenue & Minimized Denials.
We manage the entire claims lifecycle from clean claim submission to aggressive accounts receivable follow-up.
What We Deliver:
➤ Electronic claim submission
➤ Rejection management
➤ Aging AR reduction
➤ Payer communication & follow-up
Result: Faster payments & improved revenue cycle performance.
We identify root causes, correct errors then appeals to recover revenue & prevent repeat denials.
What We Deliver:
➤ Denial trend analysis
➤ Root cause correction
➤ Timely appeal submission
➤ Prevention strategy implementation
Result: Reduced Denial Rates & Recovered Lost Revenue.
Patient Payment Processing
We streamline patient billing & collections while maintaining a positive patient experience.
What We Deliver:
➤ Clear patient statements
➤ Online payment portals
➤ Payment plan management
➤ Automated reminders
Result: Higher patient collections with improved satisfaction.
We ensure your revenue cycle operations remain fully compliant with HIPAA regulations, CMS guidelines & payer-specific billing requirements.
What We Deliver:
➤ HIPAA-compliant processes
➤ Internal audit reviews
➤ Documentation accuracy checks
➤ Regulatory compliance monitoring
Result: Reduced risk & secure your revenue cycle.
Why Connexus Cure is the Ideal Revenue Cycle Management Company for You
Real-time Dashboards
Connexus Cure provides a real-time dashboard to our clients, in which you can track claim status, denials, patient balances, and cash flow.
Dedicated Account Managers
Connexus Cure has dedicated account managers, so if someone calls or emails us, they will definitely get timely updates.
Proactive alerts
Connexus Cure gives notifications about delayed payments, rejected claims, or regulatory changes.
How Our Revenue Cycle Management Process Works in Alaska
Our streamlined verification workflow ensures accuracy at every step:
#1 Patient Registration & Insurance Verification
We gather correct patient information and check insurance to avoid mistakes in claims and reduce future denials.
#2 Medical Coding & Charge Capture
We code every service correctly using the latest medical coding rules to make sure claims are processed smoothly and get the most money back.
#3 Claims Submission & Denials Managemen
We verify insurance eligibility, deductibles, copays, coinsurance, and covered services.
#4 Claims Submission & Denials Management
We send clean claims to payers and quickly fix any denied claims to get back lost money and improve cash flow.
#5 Patient Billing & Collections
We handle patient billing and collections, sending clear bills and reminders to improve patient experience and get payments on time.
#6 Payment Posting & Reconciliation
We record payments from patients and insurance companies accurately, keeping patient accounts up-to-date and easy to follow.
Connexus Cure provides customized revenue cycle management services for each specialty.
Urgent Care Revenue Cycle Management
Family Medicine Revenue Cycle Management
Cardiology Revenue Cycle Management
Internal Medicine Revenue Cycle Management
Radiology Revenue Cycle Management
Dermatology Revenue Cycle Management
Each specialty is managed with attention to its specific coding guidelines, payer policies, and reporting needs.
Connexus Cure Certifications
We strictly follow all compliance and state regulations & our certifications reflect our commitment to maintaining standards.




Connexus Cure Work With These EHRs
Our medical billing experts are familiar with every EHR system and make sure your claims are submitted accurately, no matter which one you use.








What Our Clients Say About Us
Dr. Andy *****
⭐⭐⭐⭐⭐
"Josh and the team were really good at Credentialing my new dental office. Great communication and was easy to work with."
Dr. Isaac *****
⭐⭐⭐⭐
"Connexuscure was able to file our Medicare credentialing in one day. They stayed on top of getting our lab information and let us know what was missing. They stepped us through all of the steps... We highly recommend them for Credentialing and for medical billing."
Dr. Eli *****
⭐⭐⭐⭐⭐
"Josh was very attentive and always quick with to follow up when there was a credential in issue. He always had time to take a call if/when I had a question"
Dr. Richard *****
⭐⭐⭐⭐⭐
"It was nice working with Connexus Cure Team, They are responsive and know what they are doing. I have my long pending claims settled by them in no time."
Dr. Andy *****
⭐⭐⭐⭐⭐
"Josh and the team were really good at Credentialing my new dental office. Great communication and was easy to work with."
Dr. Isaac *****
⭐⭐⭐⭐
"Connexuscure was able to file our Medicare credentialing in one day. They stayed on top of getting our lab information and let us know what was missing. They stepped us through all of the steps... We highly recommend them for Credentialing and for medical billing."
Dr. Eli *****
⭐⭐⭐⭐⭐
"Josh was very attentive and always quick with to follow up when there was a credential in issue. He always had time to take a call if/when I had a question"
Dr. Richard *****
⭐⭐⭐⭐⭐
"It was nice working with Connexus Cure Team, They are responsive and know what they are doing. I have my long pending claims settled by them in no time."
Schedule your free revenue cycle assessment in Alaska & find out about billing problems that slow down payments and decrease cash flow. Our team looks at your current process & find claim errors, denials, delays in accounts receivable (AR), and coding problems. We will give you a clear plan to improve performance.
We work with healthcare practices across Alaska to:
➤ Eliminate costly denials and underpayments.
➤ Accelerate reimbursements and stabilize cash flow.
➤ Increase first-pass claim acceptance.
➤ Reduce aging AR & recover lost revenue.
➤ Capture the full revenue your practice earns.
You will get helpful recommendations for your practice and your workflow.
Frequently Asked Questions (FAQS)
What is revenue cycle management (RCM)?
+
Revenue Cycle Management (RCM) is the financial process healthcare practices use to manage revenue, starting with appointment scheduling. It includes insurance verification, medical coding, charge capture, claims submission, payment processing, denial management, and patient collections. The goal is accurate billing, timely payments, reduced denials, regulatory compliance, and improved cash flow for medical practices.
How will your team integrate with my existing EMR/EHR system?
+
Our team works well with most EMR/EHR platforms. We carefully assess your systems to map how data moves. This ensures we can fully integrate without stopping your daily work. We move your data, create secure API connections, and train your staff. This way, our RCM solution works with your current system instead of replacing it.
What kind of reporting and visibility will I have?
+
You will have access to real-time dashboards, detailed financial reports, and performance analytics. These insights include claims status, denials, payment trends, and key financial metrics, giving you complete transparency over your revenue cycle. You can customize reports to help management make informed decisions and maximize revenue efficiency.
What is the pricing model and ROI?
+
We offer pricing options that can change. These options include paying per claim, per patient, or a subscription. We create these options to fit your organization's needs. Clients usually see a return on investment (ROI) within 3–6 months. This is because we reduce claim denials, speed up reimbursements, and improve billing accuracy. Our team gives clear projections so you can see the financial benefits of our RCM services.
How secure is my patient data with your system?
+
Patient data security is our most important concern. Our RCM services follow HIPAA and industry-standard encryption rules. This makes sure all PHI (Protected Health Information) is safe when stored and sent. We regularly check our systems, control who can access them, and constantly watch for problems to protect your data from being accessed or stolen without permission.
How quickly can we get started?
+
Our onboarding process is designed for speed and efficiency. Typically, we can begin implementation within 2 weeks, depending on the size of your organization and the complexity of your current systems. During this period, we handle workflow analysis, staff training, and system configuration to ensure a smooth transition.

